Understanding Ketoacidosis (DKA) Blood sugar: A Comprehensive Guide to Prevention and Treatment
Diabetes management is a lifelong commitment to balance. However, even with the most diligent care, certain complications can arise that require immediate medical attention. One of the most serious and potentially life-threatening conditions is Diabetic Ketoacidosis (DKA).
At Passion Health Physicians, our priority is to empower our patients with the knowledge and clinical support necessary to navigate these risks. This guide provides an in-depth look at what DKA is, how it affects your body, and the expert treatment protocols we utilize to ensure your long-term health.
What is Diabetic Ketoacidosis?
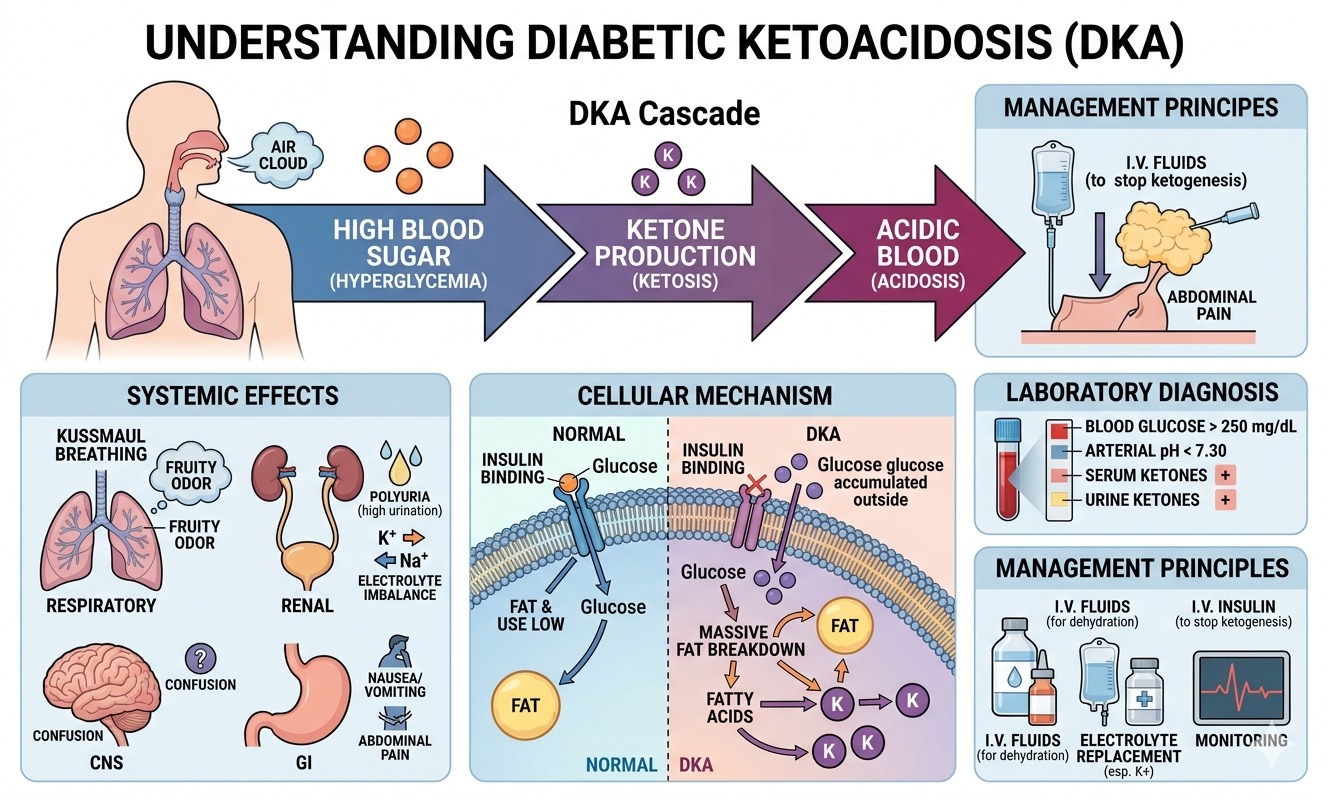
Diabetic ketoacidosis is a severe metabolic complication of diabetes, most common in individuals with Type 1 diabetes, though it can also occur in those with Type 2. It is characterized by the dangerous buildup of ketones in the bloodstream.
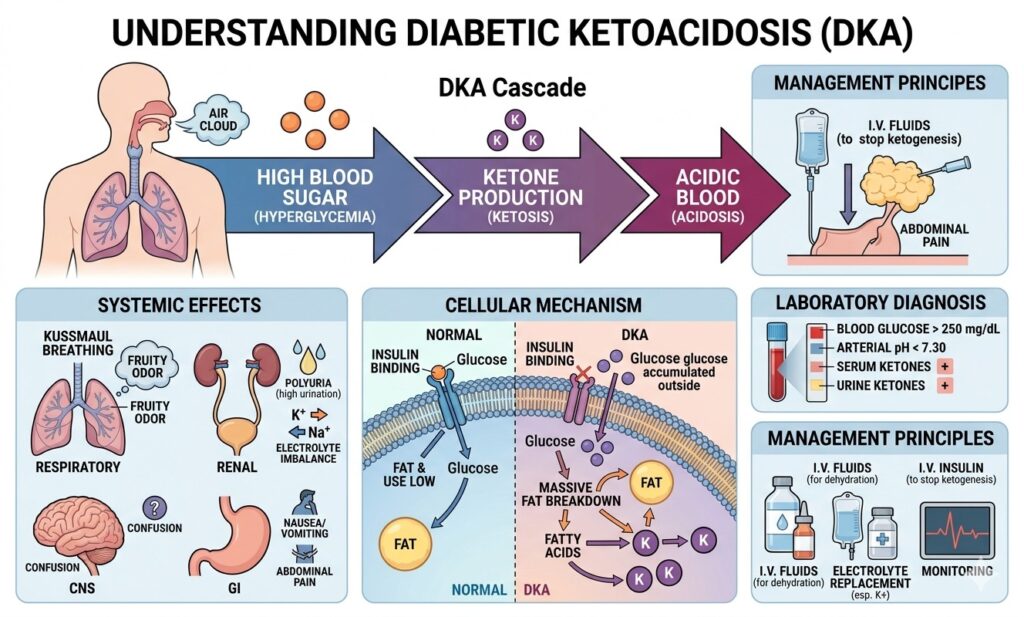
To understand DKA, we must look at how the body processes energy. Under normal circumstances, your body uses insulin to move glucose (sugar) from the bloodstream into your cells. Once inside the cells, glucose serves as the primary fuel for your muscles and tissues.
When the body lacks sufficient insulin, glucose remains stuck in the blood, leaving the cells “starving” for energy. In response, the body begins to break down fat stores at an accelerated rate. This process produces acidic byproducts known as ketones. When ketones accumulate faster than the body can eliminate them, the blood becomes acidic, leading to a state of ketoacidosis.
Recognizing the Warning Signs: Symptoms of DKA
DKA is known for its rapid onset. Symptoms can develop within 24 hours and, in some cases, are the very first indication that an individual has developed diabetes.
Early Warning Signs
If you or a loved one has diabetes, stay vigilant for these initial indicators:
Extreme Thirst (Polydipsia): An unquenchable need to drink water.
Frequent Urination (Polyuria): The body’s attempt to flush out excess glucose and ketones.
High Blood Sugar Levels: Readings consistently above your target range (typically 240 mg/dL or higher).
Fatigue and Weakness: A feeling of total exhaustion as cells fail to receive energy.
Advanced Emergency Symptoms
As the blood becomes more acidic, the symptoms become more severe and require immediate emergency intervention:
Fruity-Scented Breath: This is caused by the body attempting to exhale acetone (a type of ketone).
Nausea and Vomiting: Often accompanied by significant abdominal pain.
Shortness of Breath: Deep, rapid breathing (Kussmaul breathing) as the body tries to correct its pH balance.
Mental Confusion: Difficulty focusing or a sense of disorientation.
Root Causes: Why Does DKA Happen?
Understanding the triggers of DKA is the first step in prevention. At Passion Health Physicians, we find that most cases are linked to two primary categories:
1. Underlying Illness or Infection
When you are sick, your body releases “stress hormones” like adrenaline and cortisol. While these hormones help fight infection, they also counteract the effects of insulin. Common illnesses that trigger DKA include:
Pneumonia
Urinary Tract Infections (UTIs)
The Flu or other viral infections
2. Issues with Insulin Therapy
DKA often occurs when there is a lapse in insulin delivery. This could be due to:
Missed Doses: Forgetting an injection or failing to adjust for a high-carb meal.
Equipment Failure: A malfunctioning insulin pump or a bent infusion set.
Inadequate Dosage: Using expired insulin or insulin that has been exposed to extreme temperatures.
3. Other Contributing Factors
Physical or Emotional Trauma: High levels of stress can trigger hormone spikes.
Medical Emergencies: Heart attacks or strokes.
Medications: Certain steroids or diuretics (water pills).
Substance Misuse: Alcohol or drug use can severely disrupt metabolic balance.
Risk Factors and Potential Complications
While anyone with diabetes can develop DKA, certain individuals are at a higher risk. This includes those with Type 1 diabetes, individuals who frequently miss insulin doses, and those who lack consistent access to medical supplies.
Possible Complications
If DKA is not treated promptly, the chemical imbalance can lead to devastating consequences:
Cerebral Edema (Brain Swelling): This is particularly a risk for children and occurs if blood sugar levels are lowered too rapidly during treatment.
Hypokalemia (Low Potassium): The treatment of DKA with insulin can cause potassium levels to plummet, potentially leading to heart rhythm issues.
Hypoglycemia (Low Blood Sugar): If the transition back to normal sugar levels isn’t managed carefully, levels can drop too low.
How Passion Health Physicians Diagnoses DKA
Our diagnostic approach is thorough and data-driven. If DKA is suspected, our medical team utilizes several key tests to confirm the diagnosis and determine the severity:
Blood Glucose Testing: To measure the concentration of sugar in the blood.
Ketone Testing: Both blood and urine tests are used to check for the presence of acids.
Arterial Blood Gas (ABG): This measures the acidity (pH) of your blood.
Electrolyte Panel: We check levels of sodium, potassium, and chloride to ensure your heart and nerves can function correctly.
Additional Screenings: Chest X-rays or EKGs may be ordered to identify underlying triggers like pneumonia or heart stress.
Expert Treatment Suggestions and Clinical Management
Treatment for DKA must be performed in a clinical setting, often requiring hospitalization for close monitoring. The “Passion Health” protocol for DKA management focuses on three pillars:
Fluid Resuscitation
Dehydration is a hallmark of DKA. We administer IV fluids to replace the volume lost through excessive urination and to help dilute the excess sugar in the blood.
Electrolyte Replacement
Because DKA and its treatment can deplete essential minerals, we carefully supplement potassium, sodium, and chloride through an IV. This is vital for maintaining healthy heart function and preventing neurological issues.
Precision Insulin Therapy
Insulin is the “key” that stops the DKA process. We provide intravenous insulin to switch the body back from burning fat to burning glucose. Our team monitors your levels hourly, adjusting the dosage to ensure blood sugar falls at a safe, controlled rate.
Prevention: The Path to Long-Term Stability
Prevention is the cornerstone of the care we provide at Passion Health Physicians. We work with our patients to create a robust “Sick Day Plan” and daily management routine.
Continuous Monitoring: Check your blood sugar at least 3–4 times a day, or more frequently if you feel unwell or stressed.
Ketone Testing Kits: Always keep a urine ketone test kit at home. If your blood sugar is over 240 mg/dL and you feel sick, test for ketones immediately.
Medication Adherence: Never skip an insulin dose unless directed by your doctor.
Stay Hydrated: Drinking plenty of water helps your kidneys process excess sugar.
Expert Tip: If you notice “moderate” or “large” ketones in your urine, do not wait. Contact our office or seek emergency care immediately. Early intervention is the difference between a quick recovery and a life-threatening crisis.
Take Control of Your Health with Passion Health Physicians
Living with diabetes doesn’t mean you have to live in fear of complications. With the right team behind you, you can manage your condition with confidence and precision. At Passion Health Physicians, we offer comprehensive primary care services tailored to the unique needs of diabetic patients, from advanced health education to personalized treatment plans.
Our expert providers are dedicated to helping you stay within your target range and preventing emergencies before they start.
Ready to optimize your diabetes care?
Don’t wait for an emergency to prioritize your health. Join the Passion Health family today.